Millions of people in the United States suffer from osteoarthritis, or degenerative joint disease. The most severe cases requiring joint replacement surgery.
These replacement joints can be made of combinations of metal alloys, plastic and ceramic, but new research shows that it might be possible to regenerate damaged joints using a patient's own stem cells.
Chronic disability
Osteoarthritis is the result of infection, trauma or simply age, and is the leading cause of chronic disability worldwide.
The disease causes cartilage-protecting joint surfaces to degrade, allowing painful bone-to-bone contact. Osteoarthritis is usually treated with pain relievers and anti-inflammatory drugs, but in severe cases, the damaged joint can be replaced with an artificial one. However, this option may not work well for the growing population of younger arthritic patients.
"The average lifespan of the metal joints is about 10 to 15 years," says Jeremy Mao at the Columbia University Medical Center. "So as you can imagine, if you are say 50, 55 or younger, the surgeons will be very hesitant to place these metal joints in your body because knowing that in 10 to 15 years, there's a chance these would fail."
In order to address this concern, Mao is exploring new ways to regenerate joints.
Growing new joint cells
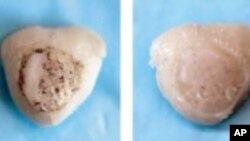
Mao replaced a portion of a rabbit's upper arm joint with a biomaterial scaffold, providing a place for cells to grow. In order to attract the rabbit's own stem cells to re-grow the cartilage, channels in the scaffold were filled with a growth factor protein.
"What we found was with one protein that we delivered in the micro-channels in the scaffolds, that was sufficient to regenerate the entire joint surface with cartilage and with bone and with blood vessels," says Mao. "So when we observe these animals with the replacement joints, what we found was there was regeneration of the entire joint that allowed the animals to resume weight-bearing and locomotion."
This return to normalcy occurred just four months after the surgical procedure, with newly grown cartilage fully covering the joint surface. When the mechanical properties of this new cartilage were tested, they showed that the regenerated cells were just as effective as the rabbit's naturally formed cartilage.
Added benefits
While human trials are still a long way off, scientists in the field are excited and encouraged by the research.
"It's absolutely necessary that we continue to push the envelope in terms of try to develop new innovative and more natural ways of effectively treating arthritis," says Dr. Mary O'Connor, chairperson of Orthopedic Surgery at the Mayo Clinic in Florida.
O'Connor says there is significant benefit to using this type of treatment for arthritis in the knee.
"When we do a knee replacement, we remove one or sometimes both of the cruciate ligaments - which are the ligaments in the center of the knee. So one of the potential advantages of this growing joint technique is perhaps the ability to preserve more of those tissues inside the knee, which would hopefully translate into more natural mechanics of the knee."
O'Connor says cost could be a factor in deciding to use this treatment. While it may not be worthwhile for older patients, younger patients are more likely to regard anything that gives them a lifelong working knee joint as well worth the cost.