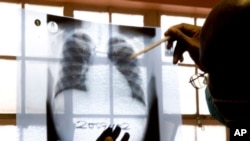
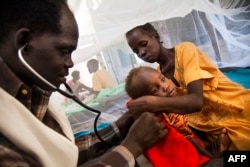
Researchers have found the number of multidrug-resistant tuberculosis cases in West Africa is greater than thought.
Officially, the World Health Organization estimates the incidence of new cases of so-called MDR-TB in the African region is 2 percent, and 17 percent among people who were treated for TB more than once.
But investigators on the ground in eight West African countries came up with higher numbers. They report that 6 percent of new cases and 35 percent of retreatment cases are drug-resistant to more than one medication.
An analysis of almost 974 sputum samples from TB patients carried out by the West-African Network of Excellence for TB, AIDS and Malaria (WANETAM), found that 39 percent were resistant to at least one first-line antibiotic used to treat tuberculosis. Additionally, bacterial isolates in 22 percent of the samples did not respond to two or more anti-TB drugs.
The findings are published in the online journal BMC Medicine.
WANETAM'S Martin Antonio, with the medical research council unit in Gambia, said the statistics are particularly worrying for the region's 245 million inhabitants who live in one of the poorest corners in the world.
"The higher the rates in the community," he explained, "the more likely it is to be spread. And we really need to catch that."
Researchers also detected the presence of what is called pre-extensively drug-resistant TB in sputum samples at all study sites in Burkina Faso, Gambia, Ghana, Guinea-Bissau, Mali, Nigeria, Senegal and Togo. These are on the verge of developing into extensively drug-resistant bacteria, which respond to neither first- or second-line drugs.
The highest proportion of pre-extensive drug resistance was seen in Ghana, in 35 percent of MDR samples. Multidrug-resistant bacteria were most prevalent among patients who'd been treated for TB before in Bamako, Mali, and Lagos, Nigeria. They were four times more likely to be resistant compared to new cases.
If the spread of MDR-TB continues at its current pace, according to Antonio, "it means the treatment options for those patients is highly limited. It means more patients may actually die from TB because they may be untreatable."
He is calling for West African governments to put aggressive, community-wide TB containment efforts in place as soon as possible to prevent a worsening of the tuberculosis epidemic.
That includes beefing up laboratories to conduct rapid testing and treatment of TB, more personnel to make sure patients take their drugs properly, and actively following those who are treated more than once for TB.