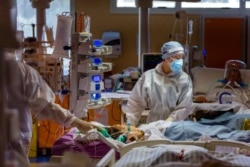
Having a cold might protect sufferers from a severe case of COVID-19, new research shows.
COVID-19 patients who had recently been infected with a common cold virus were less likely to die or require intensive care compared with those who did not have a recent cold, according to the study published recently in the Journal of Clinical Investigation.
But researchers caution that it is too early to say for sure whether past exposure to common colds helps or hinders the immune system to fight COVID-19.
COVID-19 is caused by a new coronavirus called SARS-CoV-2. But “humans have been infected with [other] coronaviruses for a long, long, long time,” said study author Manish Sagar, professor of medicine at Boston University and infectious diseases researcher at Boston Medical Center. “We have four ... coronaviruses currently that are seasonal and cause common colds.”
The question, he added, is “whether having a previous infection with common cold coronaviruses leads to any type of protection against SARS-CoV-2.”
Common colds and COVID-19
After recovering from a viral infection, the body retains a small force of antibodies and germ-fighting T cells that help protect against a second infection from the same virus.
Researchers were “kind of shocked” to find T cells that recognize SARS-CoV-2 in the blood of patients who had not been exposed to the virus, said study author Sydney Ramirez, immunologist and infectious-disease researcher at the La Jolla Institute for Immunology.
In a follow-up study, researchers showed that these T cells were left over from exposure to common cold-causing coronaviruses.
Sagar and his colleagues compared people who’d had a recent common cold infection with those who had not. They found that both groups contracted COVID-19 at the same rate, but people who had recently beaten a common cold experienced less severe COVID-19 symptoms.
“They were much less likely to require admission to the intensive care unit. And they were much less likely to die from the infection,” said Sagar.
For many adults and most children, COVID-19 causes only minor coldlike symptoms or no symptoms at all. In these people, the immune system effectively clears away virus particles and destroys infected cells, preventing serious disease.
But the “immune system is a double-edged sword,” said Andrea Cox, professor of medicine at Johns Hopkins University. Exaggerated or poorly regulated immune responses can cause inflammation that leads to breathing troubles, organ failure and death. These severe outcomes usually occur in the elderly or people with other conditions, such as obesity and diabetes.
Such vastly different responses to the COVID-19 virus could be explained, in part, by the immune system’s past experiences, experts say. Recognition of SARS-CoV-2 by preexisting T cells could enable a faster and stronger immune response and milder COVID-19 symptoms.
Common colds could worsen COVID-19
It is also possible that T cells produced from past common colds could impair the immune system’s response to COVID-19.
“We have this preexisting standing force of fighters against [disease-causing viruses], and when we encounter those [viruses], there’s expansion of that force that preexists,” said Cox. “The concern is that you might expand [a force] designed to fight something else, not designed perfectly to fight SARS-CoV-2, and that could sort of skew you down this pathway that isn’t the right path to go down.”
Prior immune experiences can be harmful in some diseases such as dengue fever. Antibodies and T cells produced in response to one version of the dengue virus can worsen the disease if they encounter a different version of the virus.
Currently, there is little evidence that T cells produced in response to common cold coronaviruses worsen COVID-19 disease, but researchers say it is too early to say that they provide protection either.
Immunity may also depend on the individual.
“Not everyone who gets infected with the virus makes exactly the same immune response. In fact, even identical twins do not make the same exact immune responses to a virus when they get exposed,” said Cox. “So, it may depend on who is being infected. And it may depend on where you are in the world, where different seasonal cold coronaviruses come in different times, and also where you have different genetic backgrounds of people being exposed.”