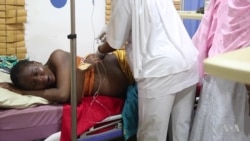
Twenty-three-year-old Radiya Ahmed Rufai is about to deliver her first child. But she has developed pre-eclampsia, a pregnancy disorder that leads to a sharp rise in blood pressure.
The doctors at Yusuf Dantsoho Memorial Hospital in the central Nigerian state of Kaduna are racing to prevent Rufai from falling into eclampsia — that’s when the pre-eclampsia advances to a level that can induce seizures.
“She was referred from another hospital to this place, with nothing to show that she was having those treatments [for pre-eclampsia]. It was here that we found out she had high blood pressure,” explains Dr. Hassan Shuaibu, a general practitioner in the hospital’s obstetrician and gynecology department.
Across Nigeria, maternal health workers are trying to improve maternal mortality. But the figures are alarming: in 2015, there were an estimated 814 maternal deaths per 100,000 live births in Nigeria, according to the World Health Organization. About half of those deaths were caused by two conditions: uncontrolled bleeding after childbirth, or postpartum hemorrhage, and pre-eclampsia.
Cultural norms
Rufai lies on the hospital bed, whimpering and shivering with pain. She’s careful not to shout out. In this part of Nigeria, cultural norms surrounding pregnancy expect women not to shout during labor — doing so would be a sign of weakness and a woman who is not able to suppress her expression of discomfort while in childbirth could face ridicule from her peers. So, women here put on a brave face, even during a difficult labor.
Rufai’s labor is getting worse. Her blood pressure is rising and her unborn infant is releasing meconium, a type of infant stool, in the amniotic fluid. It’s a telltale sign that the baby is distressed.
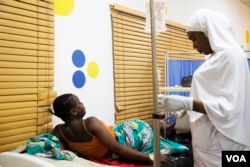
Across the ward, 32-year-old Aisha Suleiman is breastfeeding her day-old baby. It’s her seventh child. With her previous pregnancies, Suleiman experienced postpartum hemorrhaging. This delivery was no different. She lost about three pints of blood. The hospital was able to transfuse blood to her.
Lack of access to medicines
Even though, maternal mortality worldwide has decreased by nearly half in the last 15 years, Nigeria still faces a heavy burden, leading the world in the total number of maternal deaths per year. In 2015 alone, 58,000 Nigerian women lost their lives to pregnancy and childbirth-related causes.
The Nigerian Association for Reproductive & Family Health (ARFH) and the international NGO, PATH, revealed in a 2016 study how a lack of access to three basic medicines is increasing the threat of Nigeria’s two most deadly pregnancy complications: postpartum hemorrhage and pre-eclampsia/ eclampsia.
In 2012, the United Nations Commission on Life-Saving Commodities for Women and Children determined that the medicines to prevent and treat these two conditions — oxytocin and misoprostol for post-partum hemorrhage and magnesium sulfate for pre-eclampsia/eclampsia — should be made affordable and promoted for use by the global health community. But Nigerian hospitals do not always have these medicines available. And when they are available, the quality is not reliable due to poor storage and regulation.
“As of March 2016, there were 13 oxytocin products and four magnesium sulfate products registered in Nigeria that had not yet been judged to meet international quality standards. This increases the risk that maternal health products are poor or unknown,” the 2016 study reveals.
“It’s time to work hand in hand with advocates, the government, suppliers, and donors to improve the quality and availability of maternal health medicines, reduce counterfeits, and ensure that all women receive the care they deserve,” says Kehinde Osinowo, the director of programs at ARFH.
Many complications
Back at Yusuf Dantsoho Memorial Hospital, health workers are treating other complications. They’ve successfully administered magnesium sulfate to manage Rufai’s pre-eclampsia.
Sitting across from Suleiman is Hajia Muhammed in a white long hijab. She’s about to deliver twins but one of them is in a dangerous bottom-down position known as breech. Muhammed will need a cesarean section. There’s also a young woman who is HIV positive. She delivered a baby boy just hours earlier. The doctor examines him to check if the mother transferred the virus.
In the examination room, nurses scrub with antibacterial soap and hot water. They walk to the beds and kneel over women lying on their backs. Rufai waddles in and goes to a bed. The nurses want to check to see if she may be able to deliver vaginally.
The results come back negative. Her pelvis is too tight. The fetus is too stressed.
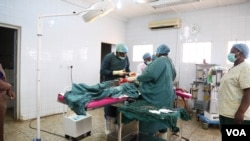
They wheel her into the operating room, with Muhammed.
Shuaibu heads the surgical team. He says that many of the Caesarean operations could be avoided with proper antenatal care.
“Most of our women don’t go for antenatal and we only see them when there are complications,” Shuaibu says. “Even if they come for antenatal, you give them medication to take, they often don’t understand why they need to take it. Poverty is another thing because they don’t have money to continue with the medication until they deliver.”
The surgeries are completed in under an hour and the women go to the recovery room. Rufai has given birth to a girl and Muhammed’s twin’s rest in the arms of elderly relatives.
The day ends at Yusuf Dantsoho Memorial Hospital’s maternity ward with no major complications.