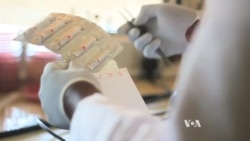
In Kenya, the rise of drug resistant bacteria could reverse the gains made by medical science over diseases that were once treatable. Kenyans could be at risk of fatalities as a result if the power in antibiotics is not preserved.
With a population of 40 million, Kenyans could be at risk from a most unlikely source. Antibiotics. In Kenya, the bacterial infections that contribute most to human diseases are often those in which resistance is most evident.
Drug resistance
Antimicrobial Resistance, or AMR, is a scientific term that means antibiotics are losing their power to cure illnesses such as pneumonia, septic wounds and malaria.
According to a 2011 analysis in Kenya by Global Antibiotic Resistance Partnership (GARP), the rise in antimicrobial resistance is a result of no new inventions of antibiotics in 25 years.
KEMRI, the Kenya Medical Research Foundation, is the national body responsible for medical research in Kenya. National studies conducted by KEMRI in collaboration with international health organizations indicate that resistance to drugs meant to treat deadly strains of bacteria that cause diseases such as dysentery had risen to as high as 100 percent.
Dr. Sam Kariuki, director of the Center for Microbiology Research at KEMRI, spoke to VOA and noted that this cross resistance is also seen in animals.
“There are farmers that use antibiotics for what we call prophylaxis for preventing disease this is one of the lead causes of developing resistance in the veterinary field, yet the same products that you find in the veterinary field are the same ones that are used in humans to a large extent,” Kariuki said.
In 2013, 254 new infections of multi-drug resistant tuberculosis were reported as a result of patients defaulting on their medications.
Loopholes also abound due to weak pharmaceutical policies that create a conducive environment for unlicensed or untrained people to sell drugs.
Inadequate pharmaceutical policies
Dr. Wilson Ndungu, a medical practitioner with JoySprings health services says that this coupled with other unscrupulous practices has exacerbated the situation.
“We can blame the willingness to enforce the policies. Either the prof, we don’t have enough manpower. We can also blame the professionals. Sometimes they prescribe [drugs] for financial gains. They prescribe antibiotics where they are not necessary and sometimes they should not prescribe even the antibiotic in cases of common cold or in case of diarrhea,” Ndunga stated.
Late last month, a global report commissioned by British Prime Minister David Cameron revealed that this resistance will claim 10 million extra lives each year and cost the global economy up to $100 trillion in the next 35 years.