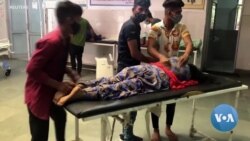
In India, the health care crisis triggered by the second wave of the coronavirus pandemic is shifting from big cities to small towns and rural areas. But as ill-equipped medical infrastructure in villages leaves people struggling to cope with the deadly virus, health experts say combating its spread in rural areas has emerged as the country’s new challenge.
In north India, people with symptoms do not go to a hospital because getting a bed is nearly impossible, according to resident Manoj Gulia. He said residents in Daryapur village, Haryana state, are fearful of reports they have seen showing conditions in hospitals — people sharing beds and shortages of medical oxygen that had battered even some of the country’s biggest hospitals earlier this month.
“There is no specialist doctor in our village so if patients come down with a fever, they just stay at home and have ayurvedic medicines,” says Gulia. Ayurveda is an ancient Indian medical tradition which some use as an alternate to modern medicine.
Prime Minister Narendra Modi has warned of the rapid spread of infection in villages. “All governments of the country are trying everything to stop this,” he said during a video conference with several chief ministers on Friday. “The awareness of people in the villages and the cooperation of village governing bodies is just as important in controlling this spread.”
While rural India was largely spared the first wave of the pandemic last year, a more transmissible coronavirus variant detected in the country and classified by the World Health organization as a variant of a global “concern,” has spread into the interiors even as infections slow in several big cities like New Delhi and Mumbai.
India has counted more than 25 million cases, but the number of new infections reported on Tuesday at 263,533, was the lowest in nearly a month. India, however, also reported its worst single day toll of 4,329.
Images of villagers relating stories of losing loved ones or tending to the sick in overwhelmed hospitals have flashed on Indian television in recent days.
Ajay Sehgal, a resident of Saifpur Firojpur village in Uttar Pradesh, one of the worst-affected states, told VOA that he rushed to get treated five hours away in Jalandhar city, where his friend owns a hospital, as he was not recovering from the infection at home. “The situation is very bad in our village. It has spread like wildfire among young and old; getting a bed is very hard and people are buying oxygen cylinders on the black market,” he says.
In Mewla Gopalgarh village in Uttar Pradesh, many people with symptoms were being treated outdoors by villagers, according to Reuters.
The government has said it will increase beds that have oxygen support in rural districts. But public health experts say upgrading health infrastructure in rural areas that have suffered decades of neglect will be a “long haul.”
“One of the key differences in rural and urban areas is that in villages, health care has mostly focused on preventive and promotive care and does not focus on treatment,” says public policy and health expert Chandrakant Lahariya. He says even testing for the virus that causes the COVID-19 disease will not be easily available to many rural residents.
Experts point out that even in big cities, well-equipped hospitals, isolation and testing centers are overwhelmed as infections rise exponentially and people and hospitals struggle with shortages of oxygen. Such facilities are missing in rural areas which are usually served by small, primary health centers that are ill-equipped to deal with the surge in infections.
“You may have some hospitals in semi-urban areas, but it is nothing close to what you have in metros in terms of sophistication of infrastructure as well as skills and capacity to deal with the virus,” according to Rajmohan Panda, professor at the Public Health Foundation of India. “Even if you have oxygen concentrators and oxygen care, people should know how to use them, and unfortunately, capacity building has not happened to that extent.”
Villages will also be hit hardest by a shortage of vaccines that is hobbling the country’s inoculation drive, experts said. Rural residents are also at a greater disadvantage because many do not have smart phones or internet access — while older people can get a jab at health centers, India has mandated that adults under 45 register on an app-based technology.
“Imagine what will happen with people in rural areas who do not have the full awareness and benefit of knowing the day-to-day changes in COVID protocols that we are being subjected to,” said Panda.
Observers warn that a slow pace of inoculations within the countryside will make it harder to counter the fury of India’s second wave.