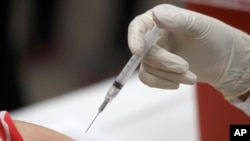
The first possible vaccine against coronavirus is on its way to human testing.
Just six weeks elapsed between when Chinese scientists released the sequence of the novel virus and when biotech company Moderna shipped its vaccine to the National Institute of Allergy and Infectious Disease to begin testing.
It's a record-breaking pace for vaccine development. Seveal other companies also are working to get their vaccines into clinical trials.
But testing a vaccine for safety and efficacy will take 12 to 18 months or more, officials say. Whatever product makes it through testing will face another hurdle: manufacturing and distributing enough vaccine to meet demand in what could be a global pandemic.
Untested tech
Moderna's vaccine is one of several candidates employing a new technology that has never been used in people.
Every vaccine until now has contained parts of the germ in question. They alert the patient's immune system to be on the lookout for the germ.
The latest vaccine from Moderna, contains only genetic instructions for those parts. The patient's own body translates those instructions into the germ parts that alert the immune system.
This kind of genetic vaccine is much quicker to produce than traditional vaccines. All scientists need to know is the germ's genetic code, which was available for the coronavirus within weeks of its discovery.
That's how Moderna can get a vaccine into clinical trials in record time.
But the 10-year-old Massachusetts-based biotech company, has never brought a vaccine to market before. If its vaccine proves safe and effective, global demand could be in the hundreds of millions or even billions of doses. The company did not respond to questions about its manufacturing capacity.
"Some of these very innovative techniques are done by very small companies who don't have experience manufacturing vaccines at the grand scale that you would need to immunize the world," said Amesh Adalja, a senior scholar at the Johns Hopkins Center for Health Security. "There will have to be some discussion about how we will develop the manufacturing capacity."
Two other small biotech companies, U.S.-based Inovio and Germany-based CureVac, are also working on gene-based vaccines.
Funders are "working to identify potential bulk manufacturers with whom to link our vaccine developers," according to the Coalition for Epidemic Preparedness Innovation, an international public-private partnership founded in 2017 to spur vaccine development for emerging diseases. All three biotech companies received funding from CEPI.
Risky business
For the companies with large-scale manufacturing experience, producing an emergency vaccine is an unwelcome business risk, experts say.
Companies "have to stop work on whatever they're working on," Adalja said. "We don't know how big the market is going to be. We don't know if (the outbreak) is going to go away (by the time a vaccine is ready) like it did with SARS. We don't know who's going to buy these vaccines."
Governments and public-private partnerships have bought vaccines in some previous outbreaks, but every case is different, and not every scenario ends well.
Several companies took financial hits while working to develop vaccines against Ebola during the 2013-2016 outbreak in West Africa.
"There's no question that a lot of them lost a lot of money trying to produce an Ebola vaccine," said Ronald Klain, who coordinated the U.S. government's response to the outbreak under President Barack Obama. Klain was speaking at an Aspen Institute event in February.
One Ebola vaccine has made it to the finish line, developed by U.S.-based pharmaceutical company Merck, with an estimated $175 million backing from the U.S. government. Health officials are using it to help contain the current outbreak in the Democratic Republic of Congo.
Vaccine maker Sanofi, meanwhile, has walked away from developing a Zika vaccine.
The French company was in negotiations in 2017 to conduct clinical trials on a Zika vaccine that the U.S. Army had developed, and to manufacture it should the vaccine prove safe and effective.
Sanofi wanted an exclusive license. But critics, including U.S. Senator Bernie Sanders, now a Democratic presidential candidate, wrote in an op-ed in the New York Times that the license would give Sanofi monopoly power and the company "will be able to charge whatever astronomical price it wants for its vaccine."
Since Sanofi had already received $43 million of U.S. taxpayer money and would receive millions more to distribute the vaccine if it worked, critics said the company should guarantee the shot would be affordable for everyone who needed it.
Sanofi and the Army did not reach an agreement, and the vaccine remains undeveloped.
Affordability and price controls
Affordability issues have already come up regarding an eventual coronavirus vaccine.
U.S. Health and Human Services Secretary Alex Azar told Congress last week, “We would want to ensure that we work to make it affordable, but we can’t control that price because we need the private sector to invest.” “
The priority is to get vaccines and therapeutics," he added. "Price controls won’t get us there.”
Azar reversed himself before Congress the next day.
"I have directed my teams that if we do any joint venture with a private enterprise, that we're co-funding the research and development program, that we would ensure there's access to the fruits of that," he said.
Even if companies and the U.S. government agree on price, the next question would be when and whether the rest of the world gets access.
“Let’s just say this vaccine is produced in the U.S.," said Seth Berkley, CEO at Gavi, the global public-private partnership that helps with access to vaccines in developing countries. "Are we going to make it available in other countries before we vaccinate the 350 million people in the U.S.? If it’s in the E.U. it’s going to be the same issue."
"Let’s say we now produce it in India for developing countries," he added during recent remarks at the Washington-based Center for Strategic and International Studies. "Well, if India’s got a big epidemic of COVID, are they going to make it available, or are they going to vaccinate their 1.3 billion people?”
Of the big international vaccine companies, only Sanofi and U.S- based Johnson & Johnson are pursuing a coronavirus vaccine. British pharmaceutical company GSK is contributing an immune-boosting ingredient to a Chinese company's vaccine candidate.
Sanofi aims to develop its product using the same system it currently uses to produce influenza vaccine and previously used to pursue a vaccine against severe acute respiratory syndrome, or SARS.
"The advantage of this approach is, first of all, you have some evidence that it will work because of the work done with SARS," said Clement Lewin at the Sanofi department dealing with U.S. government collaborations.
The company is already producing large amounts of flu vaccine, he added. "So, that means we don't have to scale up a new technology to produce (coronavirus vaccine)."
It's too soon to say what it will take to get a vaccine to everyone who needs it. The race to get a shot through clinical testing is just beginning, and manufacturing is at least a year away.
Where the epidemic will be by then is anyone's guess.