Farhad Karimi's eyes fill with tears as he recalls the events of August 1, 2017. It was a warm Tuesday evening and he was attending prayers in the Jawadia mosque in Herat, Afghanistan, along with his 18-year-old brother and a college friend. Suddenly, a large explosion forced him to the ground.
The hall of the Shi'ite mosque filled with blood. That day, the attack claimed by the Islamic State killed 33 people, wounding 65. Karimi’s brother and his classmate were among the dead.
Ever since, panic attacks and suicidal thoughts have become part of his life. Unable to cope with the trauma, he ended his studies for a medical degree and abandoned his business. For Karimi, now 26, life lost its purpose.
“Before the incident we had a private business, we imported carpets and kitchen supplies from Iran and sold them in Herat. The attack changed my life. I lost everything,” says Karimi. “I continued having nightmares about my brother, as the attack occurred in front of my eyes. I saw everything that happened.”
Decades of war and conflict have had a devastating effect on Afghanistan’s population. According to the international rights group Human Rights Watch, half of Afghans have experienced anxiety, depression or post-traumatic stress disorder.
A 2018 survey by the European Union concluded that 85% of the population have experienced or witnessed at least one traumatic event and half of the respondents experienced psychological distress. In a 2019 World Happiness Report, Afghanistan ranked as the third saddest country.
Yet, the government spends only about $0.26 per capita on mental health services. According to the 2019–2023 National Mental Health Strategy, less than 10% of the population access mental health services and there is only one psychosocial councillor for every 46,000 people.
Officials from the ministry of health did not respond to requests for a comment.
The lack of training available to mental health professionals further impedes the ability of Afghans to receive support. Other factors include the public’s poor awareness of mental health issues, stigma related to accessing mental health services, as well as poverty, exclusion and the ongoing conflict.
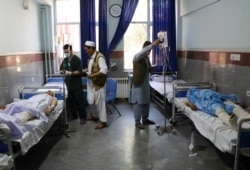
“The majority of our patients suffer from PTSD,” says Dr. Nasir Ahmad Alawi, psychiatrist at the regional hospital in Herat, which currently has 25 beds in the psychiatric ward. “We do what we can, but we don’t have enough resources. There are three million people in Herat province and we only have three counsellors.”
After multiple failed suicide attempts, Karimi decided to begin therapy and was diagnosed with PTSD. With the help of his therapist, Dr. Waheed Noorzad, he gradually managed to rebuild his life and after two-and-a-half years resumed his studies.
Encouraged by Dr. Noorzad, Karimi got involved in the work of Peace of Mind Afghanistan, a local NGO that focuses on increasing mental health awareness in the country. He soon became the head of the initiative.
“A job or a hobby is very important for everyone who attends therapy. I not only try to improve my patients’ mental wellbeing, but also support them in their lives,” says Dr Noorzad. “Some of the biggest problems of Afghans are economic so we try to help people find a job, sometimes even meet their families.”
Together with Dr. Noorzad, Karimi has been supporting those with similar experiences to his own. At a groups therapy run by the clinic, he met Ahmad Shah Rahimi, 20, who has also suffered from PTSD.
At the age of six, Rahimi saw his father being killed in revenge for an alleged insult that had taken place years earlier. It was a sunny day and the family was just returning from a picnic. Several years later, his mother died of cancer.
Rahimi and his three little brothers moved in with their maternal grandfather. While Rahimi should financially support the family as the oldest grandson, he was born with a severe visual impairment that prevents him from working at most jobs. Loneliness and a sense of failure have accompanied him most of his life.
After several suicide attempts, he decided to look for help and ended up in Dr. Noorzad’s therapy. He slowly began to open up and joined group sessions, where he met people who have been through similar experiences. His last suicide attempt was more than a year ago.
“Before I started the therapy, I had recurring nightmares because of my father’s killing, I heard terrible sounds at night and I felt extremely lonely,” says Rahimi holding Karimi’s hand. “The therapy has helped me a lot.”
But such success stories are rare. Most Afghans cannot afford pharmacological treatment, which usually accompanies therapy, as it is costly and can often take years. Since the beginning of the coronavirus outbreak some six million Afghans have lost their jobs. Eighty percent of society now lives below the poverty line. The pandemic has been a heavy burden on the cash strapped Afghan health care system and mental services are not a priority.
“Because of the coronavirus, we have more patients with anxiety disorders, phobias and obsessive-compulsive disorder. The pandemic is bolstering these issues,” says Dr. Alawi. “But we are unable to help everyone who needs support. People cannot afford treatment.”