As the world waits for a COVID-19 vaccine, scientists are testing whether shots already in use for other diseases might provide some protection from the worst impacts of the disease caused by the coronavirus.
Vaccines containing living but weakened organisms, including those against tuberculosis, polio and measles, may provide a boost to the immune system that would help fight the coronavirus.
While they probably wouldn't provide protection as good as a purpose-built vaccine, research has already shown that these immunizations help ward off diseases other than the ones for which they were designed.
Plus, these shots have a proven safety record stretching back decades.
"And not only that, it's something we can put out almost immediately," said Jeffrey Cirillo, director of the Texas A&M University Center for Airborne Pathogen Research and Imaging.
The manufacturing facilities are already up and running, delivering hundreds of millions of doses every year, he noted.
Vaccine bonus
Cirillo and his colleagues are testing whether a vaccine called BCG can help protect health workers and first responders from COVID-19.
More than 100 million children around the world receive the vaccine each year to prevent tuberculosis. But as it happens, the vaccine does much more.
When it was introduced early in the 20th century, researchers noticed steep drops in infant deaths. Some places saw up to a 50% decline, and not just from tuberculosis. Deaths from other diseases fell, too, especially respiratory diseases.
Researchers saw the same pattern over and over.
"For the last hundred years, there's all these publications showing that BCG has the ability to protect against a number of different viral infections and other bacterial infections," Cirillo said.
Others have pointed to similar benefits from live vaccines against polio and measles. In one study, 30% fewer children died after the introduction of a measles vaccine. Only 4% of those deaths were from measles.
Two-armed defenses
Live vaccines seem to act on one arm of the body's defenses.
The immune system has two parts. One, called adaptive immunity, produces antibodies that target specific germs. These provide potent, precise and long-lasting defenses against many infections.
It takes about a week to develop antibodies. Meanwhile, the second arm, innate immunity, acts as the body's first responders. The cells of the innate immune system quickly attack germs, damaged tissues, pollen — anything the body deems out of place.
Live vaccines seem to "train" cells of the innate immune system to improve their response to infections.
"What we think is that the live organisms can actually interact with these cells and then educate them so that they're a little different once they're called back out" to fight an infection, Tulane University microbiology and immunology professor Mairi Noverr said.
Experts disagree on how these cells are different. Noverr and Cirillo say these "educated" cells tamp down inflammation. If that's the case, that could help COVID-19 patients who are dying from overactive inflammation.
Others say live vaccines produce stronger innate immune responses generally, which help to protect against a broad range of infections.
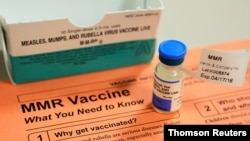
Noverr is hoping to get funding to test whether the live measles, mumps and rubella vaccine (MMR) could provide some protection against COVID-19. Others suggest testing the polio vaccine. In addition to Cirillo's, studies of BCG are under way in Australia and the Netherlands.
Given the safety record of these vaccines, "It's almost one of those things, 'Well, why wouldn't you just give it to everybody?'" Noverr said. "But you won't know (if it works) unless we do (a) double-blinded, controlled study."
That is why the World Health Organization is not recommending any of these vaccines for COVID-19 yet. Supplies are limited, WHO officials note. While tests are under way, diverting vaccines from their intended use without evidence that they help prevent COVID-19 could end up doing more harm than good.