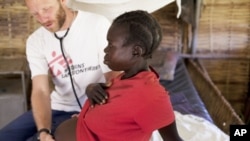
The World Health Organization recently issued new guidelines to prevent mother-to-child transmission of HIV. The recommendations include getting more women on treatment sooner and staying on it for life. The guidelines have the support of the medical aid group Doctors Without Borders, also known as MSF.
A top official for MSF says updating treatment for HIV-positive pregnant women makes a lot of sense.
“HIV in infants born to HIV-positive mothers is a big problem in the developing world. There are around 2 million HIV-positive children in developing countries, whereas in the United Kingdom, for example, there are just 70. So, we’ve almost got rid of this problem in the West, but in the developing world it’s a big problem,” said Dr. Nathan Ford, medical aid coordinator for MSF.
He said even though it would mean putting the women on antiretrovirals for life, it would actually simplify treatment in rural areas.
Start, stop and restart
“Previously, the recommendations were that women who were pregnant and HIV positive were to be given antiretroviral medicines during pregnancy, but if they did not need those medicines for their own health then once they had delivered the baby they would stop the medicines. And they would only restart the medicines if they had another pregnancy or if they fell so ill – a decline in their immune system – and then they would start the medicines for their own health,” he said.
Often the determining factor was reached when the number of CD4 immune system cells fell below 200. That’s bordering on full-blown AIDS and allows opportunistic infections to take hold. Current guidelines recommend drugs be given when the immune system is still healthy.
“These new recommendations strongly suggest that one of the options available to countries is that women who are pregnant and HIV positive start antiretrovirals irrespective of their level of immunity and continue on those antiretrovirals for life. That means that you don’t have to keep restarting and stopping and restarting,” said Ford.
Intermittent treatment could lead to drug resistance. Or treatment may not be restarted in time to protect the baby.
In the long run…..
It would require spending more money in the short term. HIV-positive pregnant women would be put on antiretrovirals sooner. But Ford takes a long-term approach.
“It’s going to save money in the long run,” he said, “because treating an HIV-positive child for life is incredibly expensive. So avoiding those infections is going to be cost-saving in the long run.”
The World Health Organization treatment update effectively puts developing countries in line with developed nations.
Ford said, “An HIV-positive person who is on antiretrovirals, those drugs suppress the virus to such a level that the person has low infectivity – a very low chance of passing on the virus to another person. So we understand a lot better now that providing treatment earlier is not only good for an individual’s health, but it’s also good for preventing the spread of the virus from one person to another. And that’s not just pregnant women. That’s any HIV-positive adult.”
The Doctors Without Borders medical aid coordinator says millions of women could benefit from the new treatment guidelines.