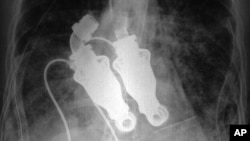
In March, two doctors at the Texas Heart Institute in Houston achieved what medical experts call a major milestone by implanting a continuous-flow artificial heart in a human patient. The mechanical heart worked flawlessly. But the patient, who suffered from other grave illnesses, eventually died after he and his family decided not to prolong treatment. The success of the artificial heart used in that case has opened the way to greater use of the device in other cardiac patients.
Since the first artificial heart was implanted in a human here in Houston in 1969, the field has advanced steadily. But it hasn't kept pace with the need for devices that can keep patients alive until they can get a real organ transplant. Heart disease remains the number one killer of Americans each year. Of the estimated 5 million people in the United States with failing hearts, only around 2,000 are likely to get a transplant this year.
That is where various types of artificial pumps have come into play. Last month, at the Texas Children's Hospital here in Houston, Jordan Merecka, 17, became the first patient in a U.S. pediatric hospital to have his congenitally deformed heart removed and replaced with an external mechanical heart pump. Meeting with reporters a few days ago, he told how he almost ran out of time, waiting to have the procedure.
"This is just a godsend. A couple months earlier and I would not be here right now," said Merecka.
Merecka, who now awaits a transplant, has limited mobility in the hospital as he remains tethered to the artificial heart beating loudly beside him.
But nearby, at the Texas Heart Institute, doctors and researchers are working with another type of artificial heart, one that is much smaller, much more efficient and does not beat.
Lead researcher Dr. Bud Frazier explained its advantages over devices like the one keeping Jordan Merecka alive at Children's Hospital.
"It is a good life-saving pump, but the limitation of it is that it is externally powered and externally driven, and it requires a large console," said Frazier. "So, if we are really going to impact the premature death from heart failure, we have to have a pump that is implantable and can replace the heart."
The artificial heart Frazier and his colleague, Dr. William Cohn, developed is small enough to be implanted in the human chest. But, unlike an animal or human heart, it produces no pulse because it is a continuous-flow mechanism. It uses a small spinning turbine to keep blood flowing at a steady rate rather than a pump that mimics the action of the heart found in humans or in the calves the doctors have used for trials.
To provide the blood flow of a natural human heart, vibrating pumps must beat 100,000 times a day, 35 million times a year, leading to mechanical breakdowns. The continuous-flow pumps are much more durable and can last years without a problem.
These continuous-flow devices have been used for some time to assist the left ventricle of the heart, which is the part that sends blood throughout the body and is the part that most often fails. But the doctors at Texas Heart Institute use a device that is essentially two such pumps put together to replace the functions of both sides of the heart.
Doctors Frazier and Cohn carried out the first successful implant of a continuous-flow artificial heart in a 55-year-old man here in Houston in March. The patient later died because of conditions unrelated to the heart operation, but Cohn says the implanted heart worked well.
"He went five weeks and his blood pressure and the flow through his body and his oxygenation was beautiful throughout that interval," recalled Cohn.
Cohn says the work he and Frazier have done shows that such a device can function much like the natural heart, even though it has no pump action to increase the pulse.
Normally when a person works or exercises, the heart beats faster so that more blood can flow to the muscles in need of energy and to the lungs where the blood is oxygenated. But Cohn says the continuous-flow heart does the same without the pulsation.
"If the conditions change so that the amount of blood arriving to the pump increases, the flow through the pump will increase," added Cohn. "It sort of has the ability to automatically increase its flow like the mammalian heart, which is, perhaps, the biggest advantage of all."
One of the biggest problems with this kind of small, implantable device is powering it without having the patient tethered to an external source of electricity. The device Doctors Frazier and Cohn developed uses small externally connected batteries that can be easily replaced without interrupting the machine's operation. But they are investigating the use of new highly efficient batteries, even ones using a tiny amount of plutonium as a power source.
Frazier says that while this may sound exotic and dangerous, the use of plutonium for such medical devices goes back to the 1970s, when they were used in heart pacemakers and studied closely.
"The thing we were concerned about was increased instance of malignancies, but we followed over a thousand of those patients over 20 years and there was no increased instance," Frazier explained. "It is bulky, though, and expensive. We came out for pacemakers with lithium-powered batteries."
Cohn says they are studying batteries that may be able to mimic the human body's natural power system. "There is a lot of other research looking at biological cells, cells that are actually powered by oxygen and glucose, much in the way the human body is," Cohn noted. "So there is a lot of battery technology that is in the works."
Since the continuous-flow artificial heart is so efficient and durable, might some future version actually work better than the heart nature has provided? Science fiction writers have speculated that one day there might be "bionic" humans, partially made up of artificial components that make them more powerful than normal people. That is something Doctors Frazier and Cohn also debate.
FRAZIER: "I don't think so."
COHN: "Well, you never know. Never try to second guess progress and human innovation. I always joke that in the 2090 Olympics there will be 'stock and modified.' You never know where it is all going to end up."
FRAZIER: "Well, we are also.. I think we are limited in time. You know, nature has had a million years or so on us in designing these things."
Doctors Bud Frazier and William Cohn are continuing their work with artificial hearts at the Texas Heart Institute in hopes of helping prevent at least some of the more than 300,000 heart disease-related deaths in the United States each year. Support for the research was provided by the National Institutes of Health as well as engineers at NASA and researchers from the University of Houston and Rice University.