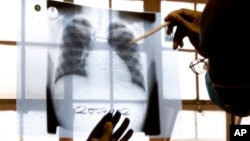
The world’s leading medical organizations are coming together to bring new Tuberculosis [TB] treatments to more than 2,600 patients in 16 countries who are diagnosed with multi-drug resistant tuberculosis [MDR-TB].
In Kenya, one clinic in Nairobi's Mathare slum is treating 48 patients suffering from MDR-TB. One of the patients suffers from the extreme-drug resistant form of the disease [XDR-TB], which requires one to be under constant injection and oral medication for a minimum of 24-months.
Home to more than half a million people, the shanty town is over-crowded. Health officials say this is a place vulnerable to an outbreak of tuberculosis.
Treatment required
Thirty-year old Elizabeth Wangechi, a Mathare resident, started feeling ill in early 2013. She started coughing, feeling chest pains and experiencing night sweats. She thought she was suffering from normal flu and believed it would go away in a matter of days or a week.
After two months without much change she went to a local clinic near her home for treatment. Wangechi said after the check-up she was diagnosed with tuberculosis.
She said at the government clinic she took medication for about four to five months, but the medications did not work and her situation worsened.
The mother of two was not responding to the medication, and four months later she was diagnosed with extreme-drug resistant TB.
According to the U.S. Centers for Disease Control, Extensively Drug-Resistant TB [XDR-TB] is a rare type of multi-drug resistant tuberculosis [MDR-TB] that is resistant to medicines normally used to treat tuberculosis and leprosy.
Wangechi said some of the medications prescribed to her for the condition were not available in the country. She said she had to wait for about a month to get the right medicines, but that she now has been under XDR medications for 10 months.
Difficult treatment
International Organizations Partners in Health [PIH], estimates 500,000 people develop MDR-TB every year, and about 10 percent of that number are XDR-TB.
Hussein Kerrow, an infectious diseases specialist with the international medical aid organization Doctors Without Borders [MSF], said after months of struggle, Wangechi responding to the new medications.
"It took us three months to get these drugs, and this drug is called Bedaquiline and is one of the new drugs that have been developed in the past 50 years," said Kerrow. "So we got the drug, she was put on new medication, we made a cocktail for her, and she did well on medication."
Kerrow said they suspect Wangechi might have caught the disease from someone who did not know about his or her TB status.
"This is an airborne disease, if you live in an overcrowded place with very little light coming in, and people don't go for TB screening, if you are living with someone who is coughing, you are likely get TB again, its an airborne disease it can be transmitted from person to person if the person is infected," he said.
Medical officials say the new drugs currently have to be combined in treatments that last up to two years. There are severe side effects, and only a 50-percent success rate for MDR-TB overall and less than 20 percent for XDR-TB.
Wangechi got 14 months to complete her dose of medicines and her three-year-old son, who also is infected got five months. She said she hopes that when she is done with her medications she will be able to go back to her teaching career or even get a better job to take care of her young family.