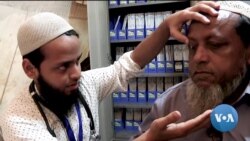
Rahim Ullah takes deep breaths as a medical assistant listens with a stethoscope to his heartbeat.
Rahim Ullah is a 62-year-old diabetic getting treatment in a refugee camp at a hospital run by Doctors Without Borders. His blood pressure, reflexes and sense of feeling in his feet are also checked.
“When I suffer from my diabetes I feel my lips are drying and feel thirsty as well as pain across my whole body,” Rahim Ullah said. “I become restless and can not sleep.”
His visit to the hospital as well as the medicine he takes home is free.
WATCH: Rohingya Crises Evolves and Medical Teams Adapt
180 medical centers
This hospital is one of about 180 medical centers that have opened since late 2017 to take care of more than 700,000 stateless Rohingya Muslims who fled to southern Bangladesh from neighboring Myanmar because of a military crackdown. U.N. investigators have said the army’s campaign had “genocidal intent.” Myanmar denies the accusations and says its security forces ran a legitimate counterterrorism operation after attacks by Rohingya militants.
The refugees now live in overcrowded camps. Toilets shared by many families can get filthy. There are times when clean water is scarce in sections of the camps, making it difficult for some refugees to even wash their hands.
“The poor living conditions in the camps are the leading cause of many multiple illnesses,” said Dr. Khalid Eltahir of the World Health Organization, “diarrhea diseases, skin diseases, respiratory infections.”
When this crisis started, there was an immediate need for emergency care for refugees with wounds from bullets and knives. There were outbreaks of measles and diphtheria that needed to be contained.
“Quick responses by the health community were necessary to keep these diseases from spreading further,” Eltahir said.
Situation stabilizes
But as the situation has stabilized, the immediate crisis has turned into a prolonged one with no signs that significant numbers of refugees will repatriate anytime soon. So medical teams are scaling up their resources to take care of refugees’ long-term health care needs. Those needs include chronic conditions such as diabetes, high blood pressure and pain.
“We assume that in the coming future there will be a big need in providing care to respond to these chronic conditions that people are living with,” said Jean-Clement Ishimwe of Doctors Without Borders.
Sixty-five-year-old Abdu Zabber says he feels pain across his body. In an examination room, a doctor checks his flexibility, how he walks and tests his hand strength.
“I feel good because they made me walk and tested my blood,” Abdu Zabber said. “They give me medicine and treat me well.”
Redistributing resources
However, health care workers say medical centers are not always distributed evenly throughout the camps, leading to concerns that refugees who are farther from health care might not get necessary treatment.
“Assessment tests are being conducted,” Eltahir of the World Health Organization said. “When they are finished we will see if we need to redistribute our resources.”