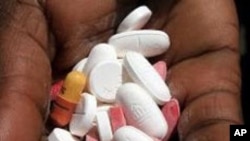
The South African government has pledged to give life-prolonging antiretroviral drugs (ARVs) to 900,000 HIV-infected people by March next year. But many of those who currently need the medicines to stay alive aren’t getting them. At some state clinics and hospitals, there are drug shortages and insufficient training for nursing staff. Staff nurses are overworked and have difficulty finding the time necessary to teach patients how to take the pills properly. This scenario is leading to serious illness and in some cases, say health professionals, to death.
South Africa’s state nurses are at the forefront of the effort to get the drugs to those who need them. But with state clinics and hospitals understaffed and poorly resourced, medical experts in South Africa say, patients’ lives are often in danger.
South Africa has the largest ARV program in the world, with hundreds of thousands of people currently receiving the medication. But many more than that are infected with HIV -- five and half million people, the largest number of any country in the world. They need ARVs if they’re to stay alive. The pills boost weak immune systems, and, if taken properly, allow HIV-infected individuals to live long and productive lives.
Waiting for relief
In Bloemfountein, the capital of South Africa’s Free State province, minibus taxis grind to a halt, leaving patients at the door of the National District Hospital.
“This is where the worst cases of HIV/AIDS come to get help,” says Sello Mokhalipi, a member of South Africa’s Treatment Action Campaign (TAC), which lobbies the government to supply ARVs to all in the country who need them.
The hospital halls ring with the piercing screams of babies and the coughs of the sick, some of them slouched against walls, staring blankly ahead, hoping for relief.
“Beds are always full here at National. As you can see, there is always a spill-over of patients into the passages,” says Mokhalipi. “The lucky ones lie on stretchers; others have benches; others must make do with the floor.”
The nearby township of Mangaung, with its population of 650,000, keeps the hospital supplied with the sick and the dying, many of them HIV-infected. South African law requires government hospitals to provide antiretroviral therapy to all who need it. But National District Hospital is one of many state facilities in the country that does not give it to all seriously ill HIV-infected people.
Medical staff members at government institutions generally refuse to speak with the media, afraid that they’ll lose their jobs. But a few senior nurses at state ARV sites in the Free State province – the epicenter of South Africa’s HIV drugs shortage – did agree to speak with VOA, on condition that their identities not be revealed.
‘A death sentence’
While the Free State health department insists that all HIV-infected patients who need ARVs get them within a matter of weeks, the nurses tell a different story.
“If patients are very sick, they have to be sent to National (District Hospital). It is a nightmare there. Patients must wait two months for treatment, sometimes longer,” one of the nurses tells VOA.
Professor Francois Venter, the president of the South African HIV Clinicians Society, says that ill HIV-infected patients must immediately be trained to use the ARVs properly and must be taking the medicines within two weeks if they’re to recover and “stay alive.”
But nurses say often they are not trained to instruct patients how to take ARVs correctly. And when they are, they don’t have the time needed to do it. At one Mangaung clinic visited by VOA, three nurses were seeing almost 200 HIV-infected patients a day.
A nurse says, “We can’t give people quality health care. We basically try to get them out of here as fast as possible.” Another tells VOA, “When you are working this fast, with this high number of people, it’s easy to make mistakes….”
Drug rationing
Because state facilities have only intermittent supplies of ARVs – and sometimes none at all -- some clinic managers order nurses to ration the drugs.
“We have the drugs, but we don’t give to everybody. We choose who to give it to. [This last year] we ran out of ARVs and we do not want this to happen again,” a manager says.
Mokhalipi explains that this situation is resulting in nurses “playing God” -- deciding which patients are “sick enough” to receive the precious medicines, when in fact all are entitled to them.
A senior nurse acknowledges that because her clinic has limited supplies of drugs, patients who visit her facility must conform to “certain criteria” before she can begin treatment. When VOA asks her to detail the criteria, she laughs uncomfortably, and responds, “I’d rather not tell you.”
Judging from this response, Mokhalipi says, it’s clear that, because of their work overload and dwindling drug stocks, the nurses are being forced to disobey a key protocol of the South African national health ministry. HIV-infected people with CD4 counts of below 200 must receive ARVs as soon as possible. A CD4 count is a measure of the strength of a person’s immune system.
“We are seeing people across the country with CD4 counts below 50 who are being refused treatment. The government clinics are getting these people onto drugs as late as possible, because they are running out of drugs,” the TAC fieldworker says.
His colleague, Thabo Nkwe, adds, “A clinic superintendent told me the same is happening with TB drugs. The clinics are always running out of TB drugs. So people are dying a lot from TB and AIDS.”
Nurses say many government ARV sites don’t even have on-site pharmacists. “This means that…nurses end up having to dispense medicine, which is against the law in South Africa, because we have not been trained in giving out medicine. So we could make mistakes, and give incorrect dosages,” one says. “But what can we do? The patients need the drugs, so we do our best.”
‘A decade of poor resource planning’
Professor Venter says even if “all the money in the world was suddenly thrown” at South Africa’s HIV/AIDS pandemic, and “all the ARVs in the world” were to be purchased, the country would still be in a dangerous situation with regard to its response to the disease. A decade of “poor human resource planning,” he maintains, has helped to create a “disaster.”
“We’ve shut down nursing colleges while we’ve had a nursing crisis developing; we don’t train enough doctors…. And this is why we’re stuck now with this disaster, which is essentially that we just don’t have enough staff to do the work.”
Venter continues, “Management of the staff is very poor. Nurses are doing jobs which are way beneath them. When they should be seeing patients, doing clinical work, they’re often engaged in bureaucratic, financial – even cleaning – duties. I’ve seen (this) in the hospitals.”
In the meantime, state nurses continue to encourage their patients to do their best to get enrolled in ARV programs managed by international NGOs, and to – in the words of one government clinic manager – “steer well clear” of state ARV sites.
Conditions are so poor at some government clinics in the Free State that international NGOs are supplying them with ARVs and equipment and are paying nurses’ salaries.
The national government has pledged an extra 900 million rands (US$ 120 million) to buy more ARVs to prevent clinics from running out of the drugs before next April.
Until then, the U.S. President’s Emergency Plan for AIDS Relief (PEPFAR) has stepped into the breach on several occasions to boost declining drug stocks -- and may well soon be asked to do it again.
Last year, it provided more than $ US 590 million in prevention and treatment programs in South Africa. PEPFAR support, according to US Government figures, has help provide antiretroviral
Treatment for over 600,0900 individuals while hundreds of thousands of HIV-positive pregnant women received antiretrovirals that will help inhibit the transmission of the virus from mothers to their unborn children. http://www.pepfar.gov/countries/southafrica/index.htm
PEPFAR is also working with the government of South Africa to achieve the goals of its National Strategic Plan, which aims to cut in half new infections within the next two years. . It also aims to provide treatment for opportunistic infections caused by HIV as well has psychological and nutritional counseling for those carrying the illness. ….