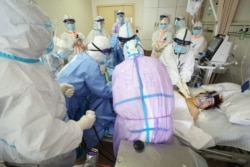
Although COVID-19 remains the same across borders---fast-moving and often fatal---how countries respond to the coronavirus may mean changing the outcome for their populations.
China imposed strict measures which have controlled the spread of the virus.
South Korea turned to testing, tracking and treating people to contain COVID-19.
The United Kingdom initially relied on herd immunity---the notion that the best way to control the outbreak was to allow the virus to spread naturally so that as more and more people became infected and built up immunity, if they survived, the outbreak would slow as the virus found fewer people to infect.
The British government pivoted hard on Monday night when Prime Minister Boris Johnson announced the closure of all nonessential shops, travel restrictions and imposed social distancing, enforced by police if necessary. The restrictions came after the government had closed schools, gyms, theaters, bars and restaurants and imposed social distancing.
As of Monday, the number of confirmed cases in Britain rose to 6,650, up from 5,683 a day earlier, and the number of deaths rose by 54, bringing the toll to 335, according to John Hopkins University data.
In all three nations, drastic times called for drastic measures.
Beijing first reported a new pneumonia emerging in Wuhan to the World Health Organization on Dec. 31. On March 18, it reported no new domestic cases. In between, it tallied some 80,000 confirmed cases and more than 3,000 deaths.
After an early cover-up, China imposed tight social controls that restricted movement, tracked individuals and even employed drones to enforce the mandatory wearing of face masks.
"At the beginning, there was a lack of information,” Chen Xi, assistant professor of public health and economics at Yale School of Public Health, told VOA Mandarin. “Therefore, when Hubei exceeded its capacity to treat patients, the government had to adopt a very aggressive disease containment policy, a comprehensive economic shutdown to prevent any new cases."
These measures imposed after Jan. 23 included the complete lockdown of many cities throughout Hubei Province including Wuhan, the construction of a modular hospital and two field hospitals to treat a patient population that overwhelmed available medical facilities. The government also imposed punishments and rewards to encourage adherence to the measures.
So far, “the policy seems to be effective, but the price is also very high,” he said. “This includes the past price and the future price. "
The past costs include what amounted to China’s complete economic shutdown. Although there has been a gradual return to normal life elsewhere, power generation in Hubei has not resumed and nearly half of the migrant workers have not returned to their jobs. Most migrant workers are employed in factories, building sites and shops far from their homes. These economic indicators show that China's economic activity is still in a semi-stagnant state more than two months into the outbreak.
At the same time, experts worry about a resurgence of COVID-19 when the lockdowns are lifted.
"We have to talk about the future cost from the perspective of immunology," Chen said.
With the lockdowns, China wanted to ensure the vast majority of people did not come in contact with the virus. Allowing free movement “will lead to a second round of infections in China if the flow of people is not well controlled down the road."
The key to South Korea's response has been widespread testing and screening. South Korea tests 15,000 people daily. The health officials have tested 250,000 people, or one in 200 South Koreans, since the first case was diagnosed on Jan. 20, some of them at drive-through stations.
WHO estimates the global mortality rate of COVID-19 at 3.4%. Yet as of March 17, the cumulative death in South Korea was 82, with a mortality rate of only 0.99%, far below the global average.
South Korean authorities use bank records, phone GPS data, and surveillance footage in their effort to locate coronavirus clusters, investigate the path of infection, quickly isolate those involved, and warn the public.
"In South Korea, health officials will perform [a] test whether you exhibit symptoms or not,” Chen said. He said the healthcare workers perform tests at random home visits and at traffic intersections.
"This actually reflects the East Asian model, which means that the government has a lot of authority. Once a person is diagnosed, he/she is strictly isolated and the chain of transmission will be monitored."
Tests are free for patients with doctor's notes, people who have recently visited China or who have had contact with a confirmed case. If a South Korean citizen just wants peace of mind, a test costs a relatively affordable $135.
Public health crisis management expert Dr. Randall Hyer was part of the WHO team that responded to the 2003 SARS outbreak. He told VOA that in South Korea, people have an incentive to get tested.
Even at the peak of the outbreak, the government made sure test kits were available. And testing made all the difference, according to Hyer, who said "Without testing, it’s the equivalent of running towards a forest full of trees with your eyes closed. You are going to hit the tree."
South Korea managed to avoid shutting down its economy and imposing the social controls China imposed.
Hyer likened South Korea to Taiwan, Singapore, Hong Kong with all of them have very similar concepts in place,” Hyer said. “One of them is early social distancing to slow the rate of spread, and then this business of testing and screening, treating people who have it, isolating them and tracing their contacts. That is how we will slow and ultimately stop the disease.”