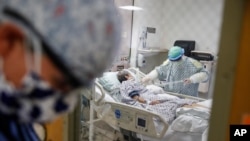
“Being in hospitals during the early days of COVID-19 was terrifying, like I was going to war. But as far as I’m concerned, those days are done,” Danielle King, a nurse working in Luling, Louisiana, told VOA.
“I think it’s pretty obvious that the pandemic was over a year ago,” she added. “The government’s lagging behind that reality, so maybe they’ll finally catch up.”
The U.S. government will take a big step in that direction Thursday as Washington officially declares an end to the coronavirus pandemic by allowing the COVID-19 Public Health Emergency (PHE) to expire.
The emergency was first instituted more than three years ago to provide funding and resources that would keep Americans safe during the then-growing global pandemic.
While many health care officials agree the time is right to end the national emergency and let state and local governments allocate resources to the COVID-19 response, some worry the move will harm Americans — particularly the impoverished — who will be less likely to afford vaccinations and risk being dropped from government programs such as Medicaid.
“It’s regrettable, but we have no certainty on what impact the PHE’s end will have on the public,” said Amy Pisani, CEO of Vaccinate Your Family, a national nonprofit organization.
“Public health advocates haven’t had a seat at the table to discuss how the end of the PHE declaration will look,” she said. “We know, for example, that COVID-19 vaccinations have been essential in keeping us safe, but how will uninsured adults access and afford the vaccines when the PHE is done? How long will free vaccines be available? Will it vary from region to region? We have no idea. All we know is it’s going to affect a lot of people.”
'No longer a threat’
The PHE was first declared in January 2020 by former Health and Human Services Secretary Alex Azar.
Since entering office in 2021, President Joe Biden has repeatedly extended the emergency. Many public health officials, including Dr. Jeffrey Elder, associate chief medical officer for emergency management at LCMC Health in New Orleans, Louisiana, believe the emergency allowed the government to take sweeping steps to support the country’s economic, health and welfare systems throughout the crisis.
“The PHE supported and funded nationwide coronavirus testing, the research and distribution of vaccinations and treatments, telehealth services, disaster responses, hospital-at-home services, nurse aide training for nursing homes and so much more,” Elder told VOA.
“And it gave our patients the comfort of knowing they couldn’t be kicked off their Medicaid insurance coverage during the emergency,” he added. “It was invaluable.”
Most public health officials, however, acknowledge the coronavirus no longer presents the crisis it once did, and the PHE may no longer be necessary.
“While we continue to see illness and deaths from COVID-19, it is no longer the threat it once was, thanks to testing, vaccines and treatment,” said Dr. Susan Kansagra, director of the North Carolina Department of Health and Human Services Division of Public Health.
She believes COVID-19 will soon be treated as routinely as other respiratory illnesses the country regularly faces.
Dr. Paul Offit, director of the Vaccine Education Center at Children's Hospital of Philadelphia, said this is a good thing.
“To call this an emergency is to elevate it above other viruses that are causing basically the same number of hospitalizations and deaths,” he said.
“I think there’s a danger to that, and I see that danger with some of my friends,” Offit said. “When their 8-year-old is sick they say, ‘Oh, I hope it’s not COVID,’ and then they test them. If they test negative, they just send them to school or to their grandparents or wherever they are going, as if it’s OK to pass on whatever disease they do have. Maybe putting coronavirus on the level of these other diseases will encourage us to take their spread all a little more seriously, as well.”
'Wide-ranging chaos’
Coronavirus cases and deaths continue to drop, but thousands of Americans are still affected by the disease. According to the Centers for Disease Control and Prevention, 1,773 people died of COVID-19 during the week ending April 5.
Some fear that with so many people still being impacted, suddenly ending the declaration could create a new set of problems.
“An abrupt end to the emergency declarations would create wide-ranging chaos and uncertainty throughout the health care system — for states, for hospitals and doctors’ offices, and most importantly, for tens of millions of Americans,” the Office of Management and Budget wrote in a Statement of Administration Policy earlier this year.
Dr. Joe McLaughlin, Alaska state epidemiologist, believes ending the PHE can reduce government spending and help the country return to a more traditional health care model. But he warns of downsides.
“We’re going to see fewer health care provider flexibilities, a reduction in access to over-the-counter tests and a decrease in some social safety net benefits. This is definitely going to affect people,” he said.
Of particular concern to health care providers is that states will no longer be forbidden from dropping enrollees from Medicaid, a federal health care program for the poor and disadvantaged, as they were during the PHE. In the months following the emergency’s conclusion, the Kaiser Family Foundation estimates that between 5.3 million and 14.2 million of America’s most vulnerable will lose their Medicaid coverage.
Additionally, it is expected that COVID-19 tests and vaccinations will no longer be offered free of charge. Once the government stops buying vaccines, the cost is expected to skyrocket. Pfizer announced it could charge as much as $130 per dose.
Challenge and opportunity
“I think it’s the right time to end it,” New Orleans nurse Brandon Legnion said of the PHE.
“I don’t think I’ve seen or heard of a single COVID-positive admission at our hospital in the last six months,” he told VOA. “The demand for PPE [personal protective equipment] and vaccines are way down, so maybe it’s time to treat coronavirus patients with the same well-researched protocols we use for other airborne transmitted diseases like tuberculosis or varicella [chickenpox].”
Ending the PHE will restructure the federal government’s COVID-19 response as an endemic, rather than a pandemic, managed through government agencies’ normal authorities. In addition to tapering coronavirus relief funds, the development of vaccines and treatments will be shifted away from federal government control.
State health department officials say the transition will be a challenge, but they are ready.
“We’ve been preparing for the possibility of the end of the federal public health emergency for some time now, and we released our state’s plan in a roadmap last year,” said AnneMarie Harper, communications director at the Colorado Department of Public Health and Environment.
“It’s a sustainable, continued response to COVID-19 that features partnerships between public and private entities that ensure all Coloradans are being taken care of, including those without insurance,” she said.
In Maryland, similar work has been done to prepare for what has become a critical transition in the country’s health care system.
Chase Cook, acting director of communications at the Maryland Department of Health, said ending the PHE makes sense because it aligns with a decrease in COVID-19 hospitalization and severity, as well as an increasing integration of coronavirus-related services into existing public health infrastructure.
“The end of the public health emergency can be seen as a challenge,” Cook told VOA, “but it’s also an opportunity ... to continue responding to the effects of the pandemic on public health, to strengthen relationships within the health care system, to maintain public-private partnerships, to grow the public health workforce, and to build on renewed efforts to decrease health disparities in Maryland. It’s an opportunity, and we’re ready.”