This is Part Four of a five-part series on health care in South Africa’s Eastern Cape province
Continue to Parts: 1 / 2 / 3 / 4 / 5
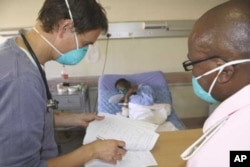
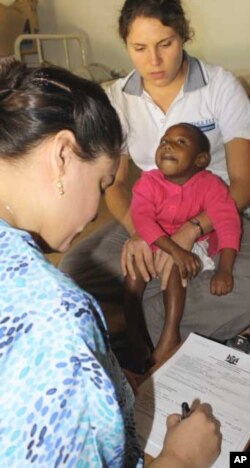
In South Africa, physiotherapists and occupational and speech therapists are playing increasingly critical roles in the survival of HIV-infected people.
But, according to one of the country’s leading rural health specialists, Dr. Ben Gaunt, their growing contribution to easing South Africa’s HIV and AIDS crisis is passing largely unnoticed.
“Allied health professionals are often invisible because they operate on the softer edges of healthcare. On the surface, their work is more about enhancing patients’ quality of life than actually saving people’s lives. But their work goes much deeper than this,” Gaunt maintained.
He continued, “Doctors can tend to be a bit arrogant and think they know everything. Actually the honest truth is allied health professionals did a four year (university) degree; they weren’t sitting around just chatting to each other. They’ve got a huge amount of practical and theoretical knowledge and what they bring to a (medical) team is incredible – and what they bring to the patient, more importantly.”
Shannon Morgan, an occupational therapist in Oliver Tambo District in South Africa’s impoverished Eastern Cape province, insisted that allied health workers should be more involved in treating HIV-infected patients.
“Our role in the care of HIV infected people is not recognized and we’re underutilized when it comes to HIV treatment. Funding comes through for this and doctors and nurses get involved in HIV projects but no one involves us,” she stated.
HIV attacks nerves
About 5.5 million people have HIV in South Africa, more than any other country. The government is giving antiretroviral (ARV) treatment to more than a million of them, but many more aren’t getting the medicine they need to bolster their weak immune systems.
As a result, they’re becoming seriously ill with infectious diseases, some of which cause severe disabilities. HIV attacks the central nervous system, sometimes causing cerebral palsy and strokes - even in children - leading to paralysis.
“With ARVs they improve and with treatment they improve, but most of the time they won’t get back to the level they were at before, and because HIV affects the brain, they can be impacted in any way – whether it be their hearing, their vision, their movements; they can be paralyzed,” Morgan explained.
Morgan’s colleague Laura Grobicki, a physiotherapist, added, “We see a lot of patients who have TB in their spine and when it affects their spine it can cause them to have spinal cord lesions. So we have quite a few members of our community who are paralyzed and will always have to use a wheelchair and will never be able to walk again, because of TB.”
Many HIV-infected South Africans also develop tuberculosis meningitis, or TB of the brain, which causes strokes. “I’d say 80 percent of the patients I see are HIV-positive, and more and more of them are tiny kids who’ve had strokes,” said Grobicki.
Dysphasia also affects about one in five people with HIV in South Africa. This condition leaves them unable to talk properly, and with a very limited ability to understand others.
Using their unique skills, therapists enable patients to function despite serious disabilities such as these.
‘Big mistake’
Gaunt insisted that allied health professionals are “crucial” to patients’ wellbeing.
At the rural state hospital where he’s head doctor, he employs five of them – including Morgan and Grobicki. But, citing budgetary constraints, most public hospitals in South Africa don’t employ a single therapist.
“At the moment in South Africa there aren’t enough therapists being trained, there aren’t enough posts, and there aren’t enough resources available for therapists,” said Grobicki.
This, said Gaunt, all adds up to a “big mistake.” He added, “I don’t think any facility can do without allied health professionals, especially in the context of HIV. Doctors are basically powerless to help stroke patients, for example. We can only sympathize with them and control their blood pressure. But therapists can teach them to walk, talk and become functional again."
This is certainly the case, but rehabilitation is always a slow process, said Grobicki. “Sometimes it’s a massive success just to get a patient to sit up for a meal. Then I help them to take their first steps with a frame, or on crutches. Then I get them to the point where they can walk on crutches by themselves outside. But it sometimes takes months to get there…”
Essential ingredient
Grobicki explained that therapists have to spend a long time with patients, when compared with doctors, but she described this as “wonderful.”
“We see them in their greatest physical and mental need, like when they can’t even stand. We get into their space,” she said. “We have to be right next to patients, our hands on their bodies, supporting them, helping them to stand up. So we get to form very special emotional and physical bonds with our patients. That’s one of the real joys of being a therapist.”
Grobicki recalled a recent visit to a hospital ward filled with men in their early 30s who were severely disabled because of HIV and TB.
“It’s incredible that they are so young, and yet so weak. I helped four of them just to sit up that day. The one guy walked, for the first time in three months. The whole room clapped for him and the doctor came and saw him and applauded him and his wife had a smile from ear to ear!”
Hope, she said, is the ingredient that’s most essential to such patients’ survival.
“It’s really important to give those kinds of patients hope, to keep them going. I tell them, ‘Even though you’re so weak now, you can start your ARVs and continue with your TB treatment and you’ll get stronger. Life isn’t over for you.’”
Hope therapy
Grobicki’s colleague, Shannon Morgan, also deals in hope.
She explained, “Occupational therapists do hope therapy. I do it with HIV-infected patients who have very low CD4 counts, of like five. They stay in hospital for a very long time. They feel very ill, very weak. These people basically just want to die.”
A CD4 count is a measurement of the strength of someone’s immune system.
Morgan continued, “I’m seeing a man now who is incredibly weak, incredibly thin. And a few days ago he was like, ‘What’s the point of living? I’m never going to walk again.’”
But Morgan pushed the patient in his wheelchair into the sun, and later encouraged him to push himself. “He did this for the first time a few days ago. And for the last two days he’s been walking to the toilet and I’ve been walking with him. I just told him he must get up and walk. Like, ‘You need to get better and you’re not going to get better if you just lie there.’ And we spoke about home and we spoke about family. Mostly I’m trying to work on his psyche and not his physical (condition) so much.”
She added, “It’s all about motivation and encouraging these people to live. Doctors can operate on people and give them medicine to make them better, but they can’t work on their attitudes. If you feel good mentally, your body feels better. If you’re feeling sad and depressed, your body will take longer to heal.”
However, Morgan acknowledged that hope therapy doesn’t always work. “Sometimes it’s too late for some patients,” she stated. “But then in a sense it’s also palliative – you’re making their last days of life as good as possible.”
Therapists not rewarded
But, despite the work that South Africa’s therapists do to ease the country’s immense HIV and AIDS burden, Morgan said they remain “under-recognized” by the health system.
Grobicki said, “Our university courses are tough to get into, and even tougher to pass. But unlike medicine and some other healthcare professions, we don’t get paid very well. So it’s difficult for particularly public health facilities to retain therapists.”
As a state physiotherapist she earns the equivalent of $1,600 a month, while Morgan gets a salary of about $2,000 as a chief occupational therapist.
“It’s crazy, hey!” Morgan said, laughing scornfully. “I can’t even afford to buy a second-hand car. I don’t even want to go live in a city because I don’t know how I’ll afford to get ahead in life. I won’t be able to afford decent accommodation.”
She added, “I love serving my country’s people, but I’ll probably end up moving overseas. It’s the old cliché – ‘health professionals leave the country; boo hoo.’ But, like, I’ve got a (study) loan that I need to pay off; I can’t pay it off working in this country.”
In the United States, according to the US Bureau of Labor Statistics, the median monthly salary for occupational therapists is almost $6,000 while for physiotherapists it’s almost $6,400.
“All therapists I know, as soon as they can they leave to work overseas. If they don’t do that, they’ll never pay their debts,” Morgan insisted. “And then the government moans and calls health professionals uncaring and unpatriotic. But, if we were paid better, we’d stay. We want to help our people, but we also need to think of our futures.”
Grobicki said only a “special kind” of person remains a therapist in South Africa’s public health sector. “You don’t get adequate financial compensation. You carry on working as a public sector therapist in South Africa because you love your patients and your work. But for some of us, love can only take you so far…”
Limited career prospects
In South Africa, therapists are able to complete “advanced therapy” degrees -- but this doesn’t mean better pay for them because no specialist therapist positions exist in the country’s state health system.
Gaunt agreed that “no really good career paths” currently exist for allied health workers in the public sector.
He explained that while public sector doctors reach a government grading of level three within 10 years, which means significantly more money for them, it takes state therapists 20 years of service to achieve the same grading.
Gaunt described this as “crazy” and added, “I don’t see how we’re going to keep therapists in the state sector at all” given this situation.
He said without the help of therapists, many disabled HIV-infected South Africans will die agonizing, slow deaths in their beds at home. But South Africa’s health system continues to leak these professionals to its well-resourced private sector, and to rich countries.
Gaunt says it’s the country’s poor disabled people who suffer most in this scenario, as they’re left without the help they need to survive.