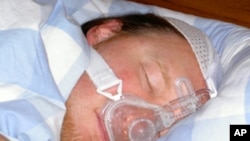
Using a breathing machine to treat sleep apnea can improve heart function and may prevent heart failure, according to British researchers.
Patients with obstructive sleep apnea stop breathing momentarily while they are sleeping.
To treat the condition, doctors sometimes prescribe a mechanical therapy known as continuous positive airway pressure, or CPAP. It uses a face mask to gently force air into the breathing passages, to keep them open.
In a new study, published online by the American Heart Association, Britain's University of Birmingham researchers used echocardiogram exams to study heart structures and function in sleep apnea patients before and after CPAP therapy, and compared their results with data on patients with high blood pressure and a healthy control group.
Gregory Lip, who led the study, said they observed heart damage in the sleep apnea patients, even though they had no overt symptoms. "Moderate to severe sleep apnea did cause significant structural and functional changes, comparable to that seen in high-blood-pressure patients."
The apnea patients were treated for an average of six months with CPAP, and then given another echocardiogram. The scan revealed that much of the heart damage had been reversed.
"CPAP therapy did reduce the thickness of the heart muscle wall," Lip said. "We showed also an improvement in the cardiac function, and also the stiffness of the cardiac chambers."
Patients with moderate to severe obstructive sleep apnea should be considered for CPAP therapy, even if they don't have any symptoms of cardiac problems, given the therapy’s apparent role in improving heart structure and function, according to Lip.
"These improvements, we hope, would be translated to a significant reduction in stroke and coronary artery disease risk," he said, "but clearly this would need to be proven in a large, prospective randomized trial."