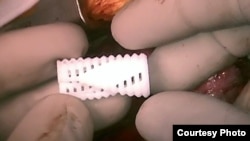
You may have heard of 3-D printing, where three-dimensional objects are “printed” by a machine that deposits a plastic-type material, usually, layer by layer, to form a solid object. Now researchers at the University of Michigan have developed what they call a 4-D medical device that is customized for very young patients and changes as their young bodies grow.
The Michigan researchers focused on children with a rare condition called tracheobronchomalacia, or TBM. The disease weakens the walls of the airway, which can collapse, starving the child of oxygen.
TBM is a devastating condition, said researcher Glenn E. Green, Maryland, of the University of Michigan. Speaking to reporters in a conference call, he said the three children in this pilot study had been hospitalized in an intensive care unit for months.
“During that time, to stay alive they required heavy sedation, narcotics, and even paralytics," he said, "They all had tracheostomies, where a breathing tube was placed through their necks, and were on artificial ventilators. There is no cure, and life expectancies for each of these children were grim.”
Patients with TBM have been treated with a splint that surrounds the airway and supports and protects it, just like a broken arm can be supported by a splint. But young children grow quickly, and the airway would soon outgrow a standard splint. So the 3-D-printed splint, customized for each patient, is designed to expand over time.
Several years after being implanted, when the airway becomes strong enough to resist collapsing, the 3-D splint is gradually absorbed by the body.
Two of the children in the study were much improved; a third suffered no complications but is still on a ventilator, presumably because of other issues.
Green says 3-D printing can help surgeons as well as patients.
“We actually printed [a replica of] the patient's airway — the trachea and bronchi — beforehand,” he explained. “By printing this ahead of time, then we were able to practice the operation before we actually incised the child just to go in and save their lives.”
Megan Frisk, an editor at the journal Science Translational Medicine, which published Green’s paper, said the findings “represent not only a new surgical option for patients suffering from obstructive airway disease, but also showing a promise for ‘4-D’-printed materials in medicine.”
The researchers are planning a larger study of this 3-D-printed splint in children with TBM.